Disorders of thyroid function, whether hyperthyroidism or hypothyroidism are medical conditions that can have a significant impact on public health, and can even shorten the lifespan of individuals of any age. Thyroid disorders, goitrous and non-goitrous forms, occur with great frequency in the adult population ranging from 0.5 to 5% in overt disease and 3 to 10% in the subclinical forms depending on the population, age and sex examined.1 While lack of dietary iodine is an important underlying cause of thyroid disorders, excess iodine, genetics and various geographical and dietary factors can also trigger thyroid disorders.2
Small aberrations in thyroid function have been associated with weight gain and blood pressure problems. 3,4,5 The elderly are most susceptible to the cardiovascular consequences of this disease, even in the subclinical or mild form which cannot be detected by clinical examination and can only be determined by biochemical tests. This underlies the importance of timely detection of thyroid disorders.
The frequency of thyroid disorders varies in different countries. A national prevalence study among the Filipino adult population using thyroid function tests will give us information vital to public health. Data on thyroid disorders, which include both overt and subclinical forms can provide estimates of the national burden of this illness. Distribution by age can help us formulate focused strategies and guidelines for improving medical care in thyroid disorders among subsets of Filipinos.
The national prevalence of goiter was first reported in 1987. Clinical examination for the presence of goiter was undertaken during the 1987 and 1993 National Nutrition Surveys allowing comparisons. There appeared to be an increase in the prevalence of goiter during this six-year period, with the initial rate in 1987 of 3.7% to 6.7% in 1993. 6. The data studied both non-pregnant and pregnant adults with the highest prevalence seen among pregnant women aged 13 to 20 years at 27.4%.
The Philippine Thyroid Diseases Study (PhilTiDeS) is the first national survey in the Philippines on the prevalence of thyroid disorders based on thyroid function tests, together with the presence of thyroid enlargement based on physical examination and iodine nutrition status of the adult non-pregnant population.
This sub-study of the PhilTiDeS aimed to determine the prevalence of thyroid dysfunction among Filipino adults using biochemical thyroid function tests according to the following categories: normal thyroid function (euthyroidism), true hyperthyroidism, subclinical hyperthyroidism, true hypothyroidism and subclinical hypothyroidism.
The second objective is to describe the prevalence of diffuse and nodular goiter in the Philippines in relation to thyroid function status.
Study Population and Sampling Design. The PhilTiDeS was conducted using the sampling design of the 7th National Nutrition Survey (NNHeS). This involved stratified sampling covering 17 regions and 80 provinces in the Philippines.
Sampling Design of National Nutrition Survey. The 7th (2003) NNS utilized the National Statistics Office (NSO) 2008 Labor Force Survey (LFS) master sample employing a stratified multi-stage sampling design in order to represent each of the 17 regions in the country. The first stage of the sampling was the selection of the Primary Sampling Units (PSUs) with probability proportional to the estimated number of households. PSUs consisted of a barangay or contiguous barangays with at least 500 households.
The second stage was the selection of Enumeration Areas (EAs) within sampled PSUs with the probability proportional to size. EAs consisted of contiguous areas in a barangay or a barangay with 150-200 households- this served as the Secondary Sampling Unit (SSU). The last stage was the selection of housing units within the sampled EAs, and this served as the ultimate sampling unit (USU). As such, the household was considered as a cluster in which all the units within a cluster were part of the survey.
The clinical and health component of the national survey in particular covered only one of the four replicates of the master sample; 25 percent of sample households were considered as sub-sample. A replicate is defined as a sub-sample that possesses the properties of the full master sample such that each replicate is able to generate national level estimates of adequate precision.
Response Rates. In the 7th NNS Clinical and Health Component, a total of 3,744 eligible households were covered from 79 provinces and 3,377 enumeration areas. The response rate obtained from interview of adults using various questionnaires was 93.7%.
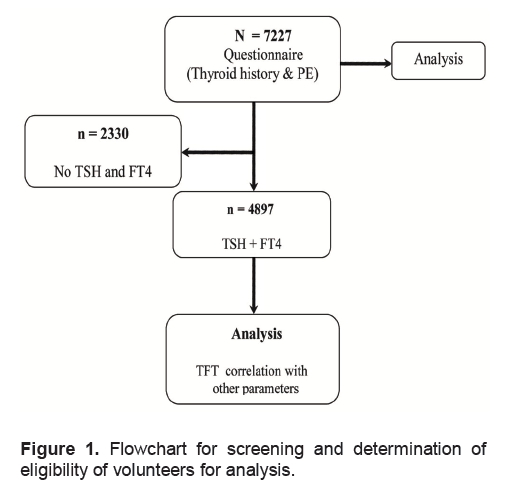
For PhilTiDes, a total of 7227 (94% response rate out of 7700 eligible volunteers) non-pregnant/ non-lactating adults aged 20 years and older were interviewed for their thyroid history and examined for goiter by trained field personnel. (Figure 1) Blood was extracted from these individuals as part of the other clinical components of NNHeS and blood samples were processed for thyroid function tests for around 5,000 individuals. The sample size for the determination of thyroid function status was calculated based on an assumed prevalence of thyroid dysfunction of 6.8% from a similar population in Taiwan 7 with an error rate of 2% at a 95% confidence level. This yields only a sample size of 608 volunteers. To be able to obtain a sample size large enough to estimate the smallest subgroup with thyroid dysfunction, that is hyperthyroidism, an assumed prevalence of 2% was used, based on previous study in Pescopagano, Italy 8 which is an area of known iodine deficiency. Using an assumed error rate of 0.4% with a 95% confidence level yielded a sample size of 4,706 rounded off to 5,000 to offset any possible drop outs or data losses. These samples comprised 68% of the eligible 7227 who had their thyroid history taken and had undergone examinations to ascertain the presence of goiter.
Non-pregnant, non-lactating adults, 20 years and older, who are currently residing in the Philippines and willing to give informed consent were included.
Click here to download Figure 1
Figure 1. Flowchart for screening and determination of eligibility of volunteers for analysis.
Training of field workers. Field workers of the NNHeS were trained by endocrinologists from the Philippine Society of Endocrinology and Metabolism (PSEM) to perform a comprehensive physical examination to determine the presence of goiter, and when a goiter is detected, to classify it according to size using the WHO-ICC IDD grading and according to morphology as nodular or diffuse goiter. They received lectures as well as individualized instructions as well as actual practice on taking a comprehensive history to uncover thyroid pathology and on proper conduct of a physical examination of the head and neck. This intensive training was done over a two-week period and they were asked to do a graded demonstration of skills at the end of the sessions.
Classification of study volunteers. Each survey volunteer underwent a structured interview to collect data on history of thyroid diseases, medications, family history and symptoms of thyroid disorders using a structured questionnaire. Afterwards the volunteers underwent a neck examination to check for the presence or absence of goiters, signs of hypo- or hyperthyroidism, and in those with goiters, the size and morphology (diffuse or nodular) of the mass. Each volunteer was then classified according to the 1994 WHO/ International Council for the Control of Iodine Deficiency Disorders (ICCIDD) palpation criteria as follows: Grade 0 is a volunteer with no goiter; grade 1 is an enlarged thyroid gland visible with neck extended or as judged from palpation; and grade 2 is a clearly enlarged thyroid with the head in normal position. 9 Thyroid or neck ultrasound was not done to verify the morphology, i.e., diffuse versus nodular goiter.
Each volunteer was also classified as either normal/euthyroid or into one of the four categories of thyroid dysfunction. These categories were defined using a combination of laboratory and clinical characteristics as follows:
1. True hyperthyroidism is defined as a TSH value of <0.47mIU/L with a high FreeThyroxine (FT4) value of >1.85 ng/dl with no intake of anti-thyroid drugs such as propylthiouracil (PTU), methimazole or carbimazole nor intake of thyroid hormones such as levothyroxine;
2. Subclinical hyperthyroidism is defined as a low TSH of less than 0.47 mIU/L with normal FT4 results, and with no intake of antithyroid drugs or thyroid hormones;
3. True hypothyrodism is defined as either:
a. An elevated TSH result >4.64 mIU/L with a low FT4 value of less than 0.71 ng/dl) with no intake of anti-thyoid drugs or levothyroxine;
b. A history of total/near total thyroidectomy or radioactive iodine ablation therapy, and currently maintained on levothyroxine therapy (regardless of TSH and FT4 result)
4. Subclinical hypothyroidism is defined as an elevated TSH greater than 4.64mIU/L and a normal FT4 with no intake of antithyroid drugs.
The reference range for normal results for TSH was 0.47 – 4.64 uIU/mL, while for the FreeT4 test it was 0.71-1.85 ng/dL. Free T 3 testing was not done nor were any thyroid auto-antibodies extracted for confirmation or determination of the etiology of the thyroid diseases.
Blood sample collection and laboratory testing. Study volunteers underwent phlebotomy by registered medical technologists to extract venous blood after 10-12 hours of fasting. The separated serum samples were frozen, placed in containers with dry ice and transported to an accredited laboratory for free T4 and TSH testing using micro-particle enzyme immunoassay by ABBOTT Diagnostics.
Laboratory procedures. Upon extraction, blood samples were processed and serum samples were immediately stored in freezers. The samples were then transported with dry ice to the designated laboratory in Manila. Upon receipt of the specimens, the laboratory staff checked the samples for adequacy and completeness of information.
Frozen specimens were thawed and numbered before processing. FT4 analysis was done using Microparticle Enzyme Immunoassay (Abbott Axsym System) with the normal reference range of 0.71-1.85 ng/dl. Third generation TSH analysis was done using Microparticle Enzyme Immunoassay (Abbott Axsym System) with the normal reference range of 0.47 – 4.64µIU/ml.
Descriptive statistics were used to summarize and analyze the results of the survey. The mean values for quantitative data, and the percentage distribution for categorical data were generated using STATA software.
A total of 4,897 persons out of the 5,000 who underwent blood extraction were included in the final analysis of the thyroid function tests. Out of 5,000 samples, 103 samples were not included because they were either inadequate or unfit for analysis. Males comprised 2302 or 47% of the population surveyed. Thyroid dysfunction was present in only 8.53% of the adult volunteers, with subclinical hyperthyroidism being the most common form of thyroid dysfunction at 5.33% followed by subclinical hypothyroidism at 2.18%, true hyperthyroidism at 0.61% and true hypothyroidism at 0.41% of adults (Table 1). The remaining 4480 (91.47%) had normal thyroid function tests.
Click here to download Table 1
Table 1. Distribution of the population based on thyroid function status, N=4897, Philippines, 2008.

Click here to download Table2
Table 2. Demographic and biochemical characteristics of the population with thyroid function tests, N=4897
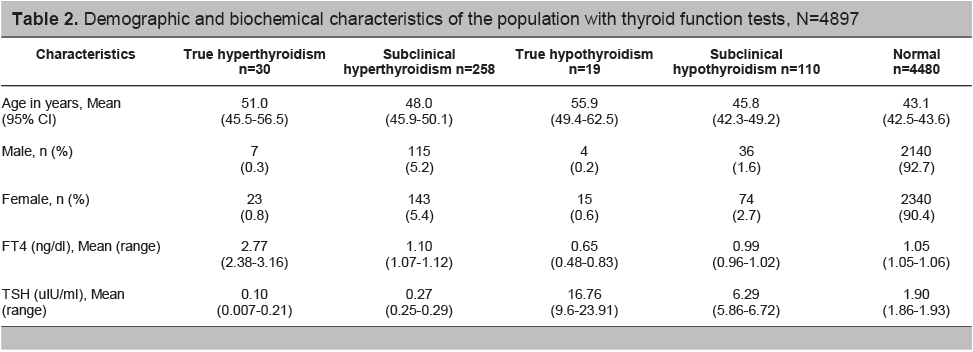
Of the 30 volunteers with true hyperthyroidism (0.61% prevalence ), 4 were taking anti-thyroid drugs at the time of the survey, comprising 0.07% of the total population surveyed. On the other hand, among the 19 volunteers (0.41% prevalence) who were labeled to have true hypothyroidism, only 2 were taking the thyroid hormone levothyroxine at the time of the survey.
Of those with subclinical hyperthyroidism, 55% are females with mean age of 48 years (95% CI 45.9-50.1 years) compared with the volunteers with normal thyroid function who were younger (mean age of 43.1, 95% CI 42.5-43.6 years).
Overall, thyroid dysfunction was more common among women, with a female to male ratio of 1.6:1. True hyperthyroidism and true hypothyroidism were 3 times more common among women than men. Persons with normal thyroid function tests (euthyroid) were younger at 43.1 years (range of 42.5 to 43.6), while those with true hypothyroidism were generally older with a mean age of 56 years (range of 49.4 to 62.5) (Table 2). Thyroid dysfunction was more common in the fifth and sixth decades of life. The TSH range for people who had normal thyroid function was 1.86 to 1.93 uIU/ml.
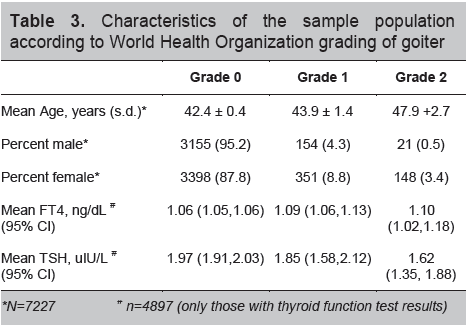
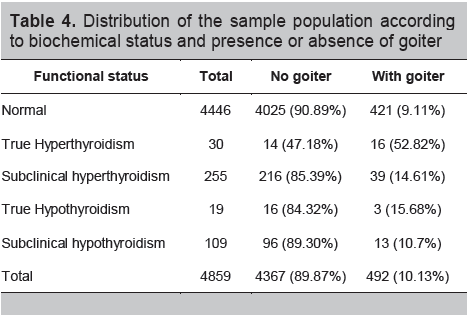
Our data also showed the correlation of thyroid dysfunction with the presence of goiter (Tables 3 and 4) using the 1994 Revised criteria of the WHO ICCIDD for grading thyroid size. Of the 7,227 volunteers who responded to the survey and were available for clinical examination, a total of 674 (or 8.9%) had goiter. Of the 674 subjects with goiters, 379 (56%) had diffuse enlargement while 295 (44%) had nodular goiter. This survey is however, limited by our inability to perform ultrasonographic verification of nodular versus diffuse enlargement. Among the 4,897 persons who further underwent thyroid function testing: 421 (9.11%) of those with normal tests present with goiter. Half of the subjects with true hyperthyroidism have goiters while only 3 (15.68%) of those with overt hypothyroidism and 13 (10.7%) of those with subclinical hypothyroidism presented with goiters.
Click here to download Table 3
Table 3. Characteristics of the sample population according to World Health Organization grading of goiter
Click here to download Table 4
Table 4. Distribution of the sample population according to biochemical status and presence or absence of goiter
This survey revealed that thyroid dysfunction is present in 8.53% of the Filipino adult population, with ages ranging between 42 and 62 years. This would translate to one out of approximately 12 adults having some degree of thyroid function abnormality. Our data shows that subclinical thyroid disorders (7.51%) are more prevalent than true or overt thyroid disorders (1.02%). Women are more affected with the different thyroid disorders, both clinical and subclinical. It is interesting that for both hyperthyroidism and hypothyroidism, the female to male ratio is almost similar at 3:1.
Our study is the first nationwide survey of thyroid dysfunction in the Philippines which took into consideration not only the clinical manifestations, but more importantly, biochemical parameters. Thyroid function tests are currently the basis for classifying thyroid dysfunction, especially since sensitive TSH assays are now able to identify people with subclinical conditions.
The prevalence of thyroid dysfunction in this Philippines survey is 8.53%, with the predominant problem being subclinical hyperthyroidism at 5.33%. A study in southern Taiwan among the elderly above 65 years old showed a prevalence rate of thyroid dysfunction of 6.8%.7 In another study looking at thyroid disease and dysfunction among adults in Norway, the prevalence of previously diagnosed hyperthyroidism was 2.5% in females and 0.6% in males, and the prevalence of hypothyroidism was 4.8% in females and 0.9% in males.10 These values are quite different from what we obtained in the Philippine population and may reflect differences in both the genetic and physical environment.
Worldwide, the prevalence of hyperthyroidism in women is between 0.5 and 2%, and is ten times more common in women than in men in iodine-replete communities. In the Whickham survey in the U.K., the prevalence of undiagnosed hyperthyroidism was 4.7 per 1000 women. 11Hyperthyroidism had been previously diagnosed and treated in 20 per 1000 women, rising to 27 per 1000 women when possible but unproven cases were included, as compared with 1.6 to 2.3 per 1000 men, in whom no new cases were found at the survey. The mean age at diagnosis was 48 years. 11 Although this data is from iodine replete areas of the world, the Philippine data appears similar with 0.61% prevalence of true hyperthyroidism (6 per 1,000) with mean age of 51 years.
A comparison of the Philippine data with surveys from iodine deficient countries shows a very different picture. The prevalence of undiagnosed hyperthyroidism in Pescopagano, an area in Italy that is considered iodine deficient, was higher, at 2%, with a further 1% of adults there having a history of toxic nodular goiter12 Approximately one-third had a diffuse goiter; the frequency in men and women was similar. In a population sample of 2656 from Copenhagen, another area of mild iodine deficiency, newly diagnosed thyrotoxicosis was found in 1.2% of women and no men, and the prevalence of known thyrotoxicosis was 1.4%.13
These comparisons make the interpretation of the results of the survey difficult, especially given the perception that many regions in the Philippines are still iodine deficient. The data on the prevalence of thyroid dysfunction will still have to be correlated with the survey on the sufficiency of iodine nutrition in the Philippines, but the low prevalence of hypothyroidism may reflect the possibility that in most areas of the country, iodine nutrition is already sufficient among the adult, non-pregnant population.
In the Philippines, the prevalence of hypothyroidism is 0.41% or 4 per 1,000. In iodine-replete communities, the prevalence of spontaneous hypothyroidism is between 1% and 2%, and it is more common in older women and ten times more common in women than in men. 11
Again, in the Whickham survey, the prevalence of newly diagnosed overt hypothyroidism was 3 per 1000 women. 11 The prevalence of previously diagnosed and treated hypothyroidism was 14 per 1000 women, versus less than 1 case per 1000 in men. One third had been previously treated by surgery or radioiodine for thyrotoxicosis. Excluding iatrogenic causes, the prevalence of hypothyroidism was 10 per 1000 women, increasing to 15 per 1000 when possible but unproven cases were included. The mean age at diagnosis was 57 years. Other studies in Northern Europe, Japan and the USA have found the prevalence to range between 0.6 and 12 per 1000 women and between 1.3 and 4.0 per 1000 in men investigated. 13
In Pescopagano, Italy, an area of mild iodine deficiency (median urinary iodine excretion 55 μg/L), the prevalence of newly diagnosed overt hypothyroidism was 0.3% of 573 women (autoimmune thyroiditis confirmed as etiology). There were no cases among 419 men and no subject had been diagnosed and treated for hypothyroidism.12 In borderline iodine-deficient Copenhagen, Denmark, 6 per 1000 of the women and 2 per 1000 men had overt but undiagnosed hypothyroidism, and 1% of all subjects were taking thyroxine. 14
For hypothyroidism therefore, our results seem closer to those countries that are iodine deficient, and yet on the other hand, the survey results for hyperthyroidism are more compatible with those of iodine replete areas. These issues can be settled once the results are connected to the data on iodine nutrition.
These results also put into focus the importance of not just the overt conditions but subclinical thyroid disorders. Thyroid dysfunction can impair an individual’s capacity to work, live well and function efficiently. Hyperthyroidism leads to a hypermetabolic state that can manifest as easy fatigability, palpitations, irritability, restlessness, sleeplessness and sweatiness. Left undetected and treated, it can lead to a potentially fatal condition, thyroid crisis manifested by heart failure, fever, cardiovascular, neurological and gastrointestinal signs. In a study among 72 patients with atrial fibrillation, 16.6% showed altered thyroid function, 6.9% with hyperthyroidism, 5.6% with hypothyroidism and 4.2% with elevated T4 due to amiodarone. 15
Hypothyroidism can lead to coma, heart failure and mental impairment causing loss of memory a treatable condition. Disastrous results can be averted by proper detection and treatment.
Minor degrees of thyroid dysfunction that may seem inconsequential may lead to dire consequences in vulnerable patients such as those with cardiovascular disease and the elderly. Subclinical hyperthyroidism can lead to disturbances in bone metabolism and cardiac function such as atrial fibrillation. Individuals on levothyroxine with subclinical hyperthyroidism who were studied using Doppler echocardiography and 24 hour Holter electrocardiogram monitoring showed increased 24 hour mean heart rate and supraventricular arrhythmia, left ventricular mass index, higher rate of systolic function and impairment of diastolic dysfunction.16 A low serum TSH concentration is generally a sensitive marker of thyroid hormone excess and has been reported in a large population-based study to be associated with a 3-fold higher risk of developing atrial fibrillation (AF) in the subsequent decade.17 The cumulative incidence of AF after 10 years among subjects with a low TSH concentration ( 0.1 mU/liter) was 28%, compared with 11% in those with a normal TSH (p = 0.005). The presence of atrial fibrillation predisposes to embolic events which may contribute to increased vascular mortality among patients with excess thyroid hormones. Perhaps, the most deleterious effect of subclinical hyperthyroidism is that it predicts future risk of development of overt hyperthyroidism.
Subclinical hyperthyroidism appears to pose more problems for the elderly and has been particularly well-studied in this population. It is associated with a higher mortality rate in chronically-ill geriatric patients (62% versus 28%, p <0.05) and poses a 2.2-fold risk in mortality from all causes and 3-fold risk of cardiovascular death among those aged more than 60 years old after a single measurement of low TSH.17 These studies support the recommendations on screening for thyroid dysfunction and treatment of subclinical hyperthyroidism among the elderly. 18,19
Subclinical hypothyroidism has been associated with dyslipidemia that can lead to cardiovascular disease. Detection and correction can correct its consequences and improve health.
Knowledge of this data should be able to help our government policy makers, health insurance policy makers and individual health practitioners to make the necessary steps to address the thyroid dysfunction of our many
The national prevalence of thyroid dysfunction among adults in the Philippines is 8.53%. Subclinical hyperthyroidism and subclinical hypothyroidism are the most common thyroid dysfunctions with prevalence rates of 5.33% and 2.18% respectively; while 0.6% present with true hyperthyroidism and 0.4% present with true hypothyroidism. Among the adult Filipino population, 8.9% have goiters by physical examination. Half of the hyperthyroid patients have goiter, while 1 out of 6 to 10 patients with other types of thyroid dysfunction have goiter.
The PhilTiDeS research team is grateful for the invaluable contribution of the following:
Dr. Mario Capanzana of FNRI, Ms Corazon Cerdena of FNRI, Merck Inc, Abbott Pharmaceuticals, Pharmalink-Invida, MSD-Schering Plough and the Philippine Council on Research and Development.
1. Helfand M, Redfern C. Screening for Thyroid Disease : An update . Annals of Intern Med 1998;129, 144-158.
2. Knudsen N, Laurberg P, Perild H. Risk factors for goiter and thyroid nodule. Thyroid. 2002; 12: 879-88.
3. Knudsen N, Laurberg P, Rasmussen LB et al. Small differences in thyroid function may be important for body mass index and the occurrence of obesity in the population. J Clin Endocrinol Metab. 2005; 90:4019-24.
4. Gumieniak O, Perlstein TH, Hopkins PN et al. Thyroid function and blood pressure homeostasis in euthyroid subjects. J Clin Endo and Metab. 2004; 89:3455-61.
5. Asvold BO, Bjoro T, Nilsen TI et al Association of blood pressure with TSH in the reference range:A population based study. J Clinic Endo and Metab 2007; 92: 841-45.
6. Philippine Nutrition Facts and figures, 2001.
7. Chia-Chang Chuang, Shan-Tair Wang, Pei-Wen Wang, Mei-Lin Yu . Prevalence Study of thyroid dysfunction in the elderly of Taiwan. Gerontology. 1998;44:162-167
8. Parle JV, Maisonneuve P, Sheppard MC, Boyle P, Franklyn JA. Prediction of all cause and cardiovascular mortality in elderly people from one low serum thyrotropin result: A 10-year cohort study. Lancet. 2001; 358: 861-865.
9. WHO, UNICEF & ICCIDD. Indicators for assessing iodine deficiency disorders and their control through salt iodization. WHO/NUT/94.6. Geneva: WHO 1994.
10. T. Bjuro, J Holmen, eKruEger, K Midthjell, K Hunstad, T Schreiner, et al.Prevalence of thyroid disease, thyroid dysfunction and thyroid peroxidase antibodies in a large, unselected population. The health study of Nord-Trundelag (HUNT). European Journal of Endocrinology. 2000; 143; 639-64
11. Tunbridge WMG, Evered DC, Hall R, Appleton D, Brewis M, Clark F, Evans JG, Young E, Bird T, Smith PA. The spectrum of thyroid disease in the community: The Whickham survey. Clin Endocrinol 1977; 7:481-493.
12. Aghini-Lombardi F, Antonangeli L, Martino E, Vitti P, et al. The spectrum of thyroid disorders in an iodine-deficient community: The Pescopagano Survey. J Clin Endocrinol Metab 1999; 84:561-566
13. Vanderpump MPJ. The epidemiology of thyroid diseases. In: Braverman LE, Utiger RD, eds. Werner and Ingbar's The Thyroid: A Fundamental and Clinical Text. 2005.
14. Knudsen N, Jørgensen T, Rasmussen S, Christiansen, Perrild H. The prevalence of thyroid dysfunction in a population with borderline iodine deficiency. Clin Endocrinol 1999; 51:361-367.
15. Barbisan JN, Fuchs FD, Schaan BD, Prevalence of thyroid dysfunction in patients with acute atrial fibrillation attended at a cardiology emergency room. Sao Paulo Med J. 2003;121:159-62
16. Biondi B, Fazio S, Palmieri EA, et al. Effects of chronic subclinical hyperthyroidism from levothyroxine on cardiac morphology and function. [Effetti dell'ipertiroidismo subclinico cronico da terapia con levotiroxina su morfologia e funzione cardiaca]. Cardiologia 1999;44(5):443-9.
17. Kovacs G et al. Subclinical hyperthyroidism and mortality rate in geriatric patients. The Thyroid and Cardiovascular Risk: Merck European Thyroid Symposium Berlin 2004, June 10-13.
18. Sawin CT, Séller A, Wolf PA, Belanger AJ, Baker E, Bacharach P, et al. Low serum thyrotropin concentrations as a risk factor for atrial fibrillation in older persons. NEJM 1994; 331(19): 1249-1252.
19. Volzke H, Schwahn C, Wallaschofski H, Dorr M. The relation of thyroid dysfunction with all-cause and circulatory mortality: Is there a causal relationship? J Clin Endocrinol Metab. 2007 May 1.
Articles and any other material published in the JAFES represent the work of the author(s) and should not be construed to reflect the opinions of the Editors or the Publisher.
Authors are required to accomplish, sign and submit scanned copies of the JAFES Declaration that the article represents original material that is not being considered for publication or has not been published or accepted for publication elsewhere.
Consent forms, as appropriate, have been secured for the publication of information about patients; otherwise, authors declared that all means have been exhausted for securing such consent.
The authors have signed disclosures that there are no financial or other relationships that might lead to a conflict of interest. All authors are required to submit Authorship Certifications that the manuscript has been read and approved by all authors, and that the requirements for authorship have been met by each author.