Predictors of Response to Therapy among Post Thyroidectomy Adult Filipino Patients with Papillary Thyroid Carcinoma based on the 2015 American Thyroid Association Guidelines
DOI:
https://doi.org/10.15605/jafes.036.02.18Keywords:
papillary thyroid cancer, response to papillary thyroid cancer therapy, well-differentiated thyroid cancerAbstract


*Visual Abstracts prepared by Dr. Carmen Carina Cabrera
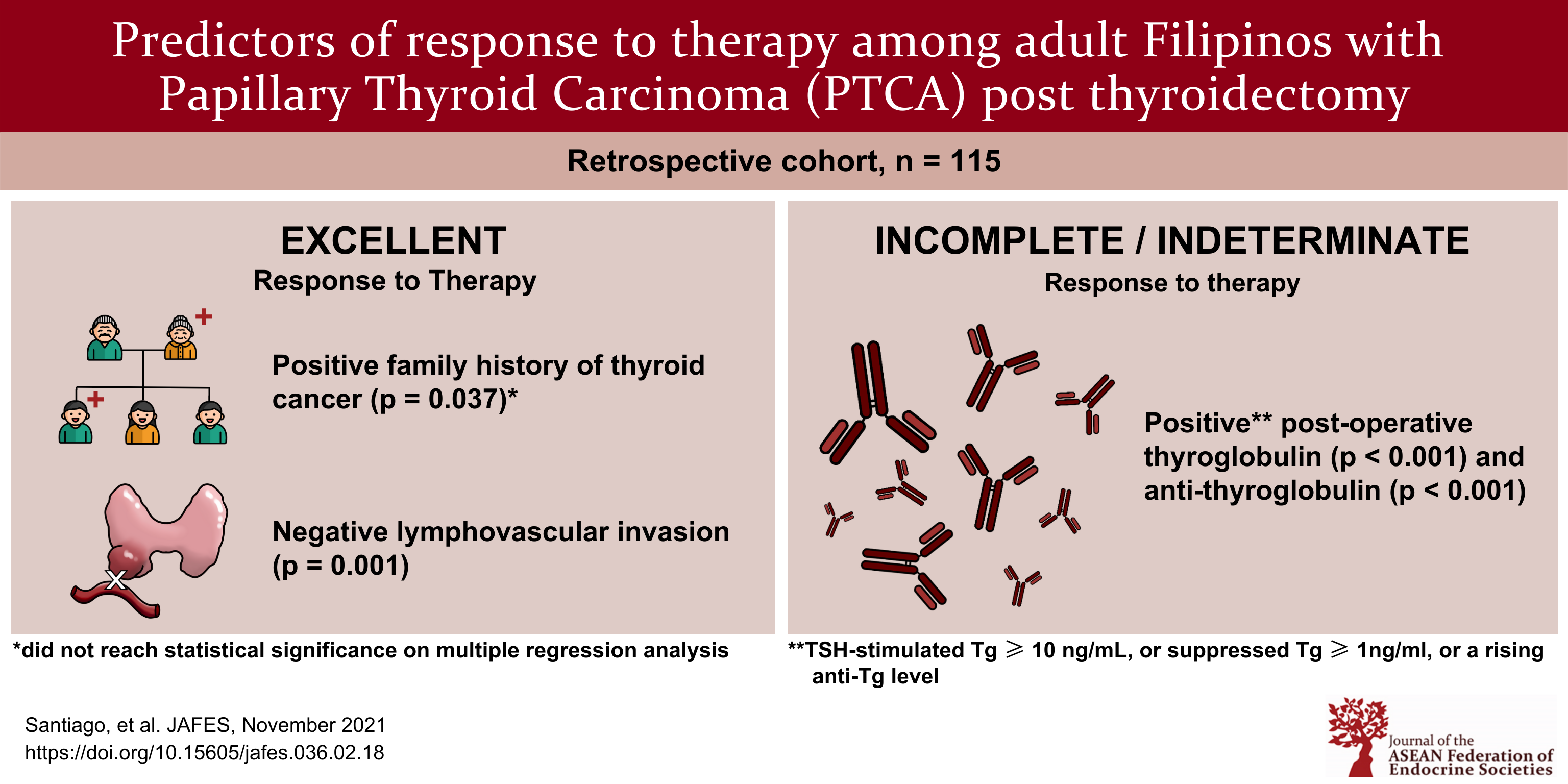
Objective. To identify factors independently associated with incomplete response to therapy based on the 2015 ATA guidelines in surgically treated Filipino patients with papillary thyroid carcinoma (PTC).
Methodology. This is a retrospective cohort study of adults aged 21-74 years with papillary thyroid carcinoma (PTC) treated with surgery with or without radioactive iodine therapy (RAI) in Makati Medical Center from 2013 to 2017. We collected the following factors through a review of charts: age at diagnosis, gender, family history of thyroid cancer, date of surgery, tumor size, capsular/lymphovascular invasion, lymph node/distant metastases, stage, risk of recurrence, dose of post-surgical RAI therapy, initial post-treatment serum Thyroglobulin (Tg) and anti-Tg antibody levels (Negative Tg level: suppressed non-stimulated Tg <0.2 ng/mL or TSH-stimulated Tg <1 ng/mL; Positive Tg level: suppressed Tg >1 ng/mL or a TSH-stimulated Tg >10 ng/mL or rising anti-Tg antibody levels), thyroid stimulating hormone suppression, post-operative imaging studies and levothyroxine dose. Response to therapy was checked 6-24 months post-therapy.
Results. We analyzed a total of 115 patients with PTC who underwent thyroidectomy. Patients who had family history of thyroid cancer were less likely to have an incomplete or indeterminate response (p=0.045). None of the patients with excellent response had lymphovascular invasion. Having a positive Tg (p=0.001) and positive anti-Tg postoperatively (p<0.001) were strongly associated with incomplete or indeterminate response.
Conclusion. Patients who were positive for thyroglobulin and anti-thyroglobulin post-operatively were strongly associated with incomplete or indeterminate response to therapy in PTC.
Downloads
References
Alvarado R, Sywak MS, Delbridge L, Sidhu SB. Central lymph node dissection as a secondary procedure for papillary thyroid cancer: Is there added morbidity? Surgery. 2009;145(5):514-8. https://pubmed.ncbi.nlm.nih.gov/19375610. https://doi.org/10.1016/j.surg.2009.01.013.
Ries LAG, Melbert D, Krapcho M, et al (eds). SEER Cancer Statistics Review, 1975-2004. National Cancer Institute. Bethesda, MD. https://seer.cancer.gov/csr/1975_2004/, based on November 2006 SEER data submission, posted to the SEER web site, 2007.
Haselkorn T, Bernstein L, Preston-Martin S, Cozen W, Mack WJ. Descriptive epidemiology of thyroid cancer in Los Angeles County, 1972-1995. Cancer Causes Control. 2000;11(2):163-70. https://pubmed.ncbi.nlm.nih.gov/10710201. https://doi.org/10.1023/a:1008932123830.
Kus LH, Shah M, Eski S, Walfish PG, Freeman JL. Thyroid cancer outcomes in Filipino patients. Arch Otolaryngol Head Neck Surg. 2010;136(2):138-42. https://pubmed.ncbi.nlm.nih.gov/20157058. https://doi.org/10.1001/archoto.2009.206.
Lo TE, Uy AT, Maningat PD. Well-differentiated thyroid cancer: The Philippine General Hospital experience. Endocrinol Metab (Seoul). 2016;31(1):72-9. https://pubmed.ncbi.nlm.nih.gov/26754584. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4803565. https://doi.org/10.3803/EnM.2016.31.1.72.
Horn-Ross PL, McClure LA, Chang ET, et al. Papillary thyroid cancer incidence rates vary significantly by birthplace in Asian American women. Cancer Causes Control. 2011;22(3):479-85. https://pubmed.ncbi.nlm.nih.gov/21207130. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3291661. https://doi.org/10.1007/s10552-010-9720-5.
Gomez SL, Noone AM, Lichtensztajn DY, et al. Cancer incidence trends among Asian American populations in the United States, 1990-2008. J Natl Cancer Inst. 2013;105(15):1096-110. https://pubmed.ncbi.nlm.nih.gov/23878350. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3735462. https://doi.org/10.1093/jnci/djt157.
Haugen BR, Alexander EK, Bible KC, et al. 2015 American Thyroid Association management guidelines for adult patients with thyroid nodules and differentiated thyroid cancer: The American Thyroid Association guidelines task force on thyroid nodules and differentiated thyroid cancer. Thyroid. 2016;26(1):1-133. https://pubmed.ncbi.nlm.nih.gov/26462967. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4739132. https://doi.org/10.1089/thy.2015.0020.
Mendoza ES, Lopez AA, Valdez VAU, et al. Predictors of incomplete response to therapy among Filipino patients with papillary thyroid cancer in a tertiary hospital. J Endocrinol Invest. 2016; 39(1):55-62. https://pubmed.ncbi.nlm.nih.gov/26036600. https://doi.org/10.1007/s40618-015-0319-2.
Tuttle RM, Tala H, Shah J, et al. Estimating risk of recurrence in differentiated thyroid cancer after total thyroidectomy and radioactive iodine remnant ablation: Using response to therapy variables to modify the initial risk estimates predicted by the new American Thyroid Association staging system. Thyroid. 20(12):1341-9. https://pubmed.ncbi.nlm.nih.gov/21034228. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4845674. https://doi.org/10.1089/thy.2010.0178.
Amin A, Badwey A, El-Fatah S. Differentiated thyroid carcinoma: An analysis of 249 patients undergoing therapy and aftercare at a single institution. Clin Nucl Med. 2014;39(2):142- 6. https://pubmed.ncbi.nlm.nih.gov/24368533. https://doi.org/10.1097/RLU.0000000000000324.
Sciuto R, Romano L, Rea S, Marandino F, Sperduti I, Maini CL. Natural history and clinical outcome of differentiated thyroid carcinoma: A retrospective analysis of 1503 patients treated at a single institution. Ann Oncol. 2009;20(10):1728-35. https://pubmed.ncbi.nlm.nih.gov/19773250. https://doi.org/10.1093/annonc/mdp050.
Palme CE, Waseem Z, Raza SN, Eski S, Walfish P, Freeman JL. Management and outcome of recurrent well-differentiated thyroid carcinoma. Arch Otolaryngol Head Neck Surg. 2004;130(7):819-24. https://pubmed.ncbi.nlm.nih.gov/15262757. https://doi.org/10.1001/archotol.130.7.819.
Wang LY, Ganly I. Nodal metastases in thyroid cancer: Prognostic implications and management. Future Oncol. 2016; 12(7): 981–94. https://pubmed.ncbi.nlm.nih.gov/26948758. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4992997. https://doi.org/10.2217/fon.16.10.
Matthews TJ, Chua E, Gargya A, Clark J, Gao K, Elliot M. Elevated serum thyroglobulin levels at the time of ablative radioactive iodine therapy indicate a worse prognosis in thyroid cancer: An Australian retrospective cohort study. J Laryngol Otol. 2016;130(Suppl. S4):S50-3. https://pubmed.ncbi.nlm.nih.gov/27488338. https://doi.org/10.1017/S0022215116008331.
Spencer CA. Challenges of serum thyroglobulin (Tg) measurement in the presence of Tg autoantibodies. J Clin Endocrinol Metab. 2004;89(8):3702–4. https://pubmed.ncbi.nlm.nih.gov/15292292. https://doi.org/10.1210/jc.2004-0986.
Espiritu GAM, Malana JT, Dumasis AJGV, Ang DC. High preponderance of BRAF V600E mutation in papillary thyroid carcinoma among Filipinos: A clinicopathologic study. J Glob Oncol. 2019;5:1-6. https://pubmed.ncbi.nlm.nih.gov/30694737. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6426509. https://doi.org/10.1200/JGO.18.00085.
Published
How to Cite
Issue
Section
License
Copyright (c) 2021 Aivind Gabrielle Santiago, Maria Jocelyn Isidro, Joseph Parra

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.
The full license text is available at: http://creativecommons.org/licenses/by-nc/3.0/legalcode.
To request permission to translate, reproduce, download, or use articles or images for commercial reuse or business purposes from the Journal of the ASEAN Federation of Endocrine Societies (JAFES), kindly complete the Permission Request for Use of Copyrighted Material Form and email jafes@asia.com or jafes.editor@gmail.com.
A written agreement will be issued to the requester once permission has been granted.












